Fistulas may form in many parts of the body. A fistula is an abnormal connection or tunnel between two organs in the body or between an organ and your skin.
ABOUT PELVIC FISTULAS
Fistulas start because of damage to the tissue. As the tissue damage worsens, healthy tissue dies off. This can cause a new connection (fistula) to form between two spaces in that area. Depending on the cause or seriousness of the tissue damage, a fistula may form within days, weeks, months, or over years.
A small number of women are born with a fistula. For others, causes of fistulas in the pelvic area can include:
- Childbirth: Very long periods of labor may result in a breakdown of pelvic tissue. The damaged tissue may cause a fistula to form. In addition, both tearing of the skin and/or underlying muscles of the perineum during vaginal delivery (perineal tears) and Cesarean sections increase a woman’s risk for fistulas.
- Surgery: Fistulas are a rare complication of different types of pelvic surgery. For example, a fistula may happen after a hysterectomy or pelvic reconstructive surgery.
- Cancer: Cancer in the pelvic area or radiation used to treat cancer may damage tissue. If the damage worsens, a fistula may form.
- Pelvic injury: Other damage to the pelvic organs increases your risk of developing a fistula. In rare instances, leaving a pessary or diaphragm in for too long can lead to tissue damage, which may cause a fistula to form.
- Chronic bowel conditions: Diverticulitis or inflammatory bowel disease (such as Crohn’s disease or ulcerative colitis) may develop fistulas that involve the bowel and vagina or nearby skin.
GENITOURINARY FISTULAS
Genitourinary fistulas are abnormal connections between the vagina or uterus and some part of the urinary system, including the urethra, bladder, or ureter. The tunnel-like fistula allows urine to flow into the vagina or uterus, creating constant urine leakage.
Genitourinary fistulas increase your risk for urinary tract and kidney infections. If urine seeps into the abdomen, women can experience bloating and pelvic pain, nausea and vomiting, and a poor appetite. Other symptoms include:
- The constant flow of urine from your vagina, although some women have only occasional leakage.
- Urine odor from the vagina.
- Skin problems near the vaginal opening because of constant wetness.
DIAGNOSIS OF GENITOURINARY FISTULAS
Your medical provider will ask you about your symptoms and when they started. If you have had surgery before, it is helpful to get the operative report to know exactly what was done.
A thorough pelvic exam will be performed to look for the source of the urine leakage. Sometimes various dyes are used to determine where the fluid is leaking from. For the double dye test, you take a pill that turns your urine orange. In addition, the provider inserts a blue dye into your bladder. Then, you put a tampon in your vagina:
- If the tampon turns blue, the fistula may be between your vagina and your bladder, known as a vesicovaginal fistula.
- If the tampon turns orange, the fistula may involve your ureter and the vagina, known as a ureterovaginal fistula.
You may undergo other tests as well:
- Cystoscopy: A small telescopic camera is inserted into your bladder and urethra to look for the fistula’s location and size. This can be done in the office without general anesthesia.
- Imaging tests: This may include a computerized tomography (CT) scan specialized to examine the urinary tract; or a specialized x-ray, called a retrograde pyelogram.
- Lab work: A urine test may be done to check for a urinary tract infection. Blood tests may be needed to check kidney function and for signs of infection.
TREATMENT OF GENITOURINARY FISTULAS
The size and location of the genitourinary fistula will determine your treatment options. For very small fistulas, placement of a urethral catheter for 4 to 6 weeks to drain urine from the bladder may heal the fistula. If the fistula involves the ureter, placing a thin, hollow tube into the ureter (called a stent), will allow urine to drain from the kidney to the bladder. Both of these stop the urine from flowing through the fistula, allowing it to close.
If those options do not work or the fistula is too large, surgery is required. Fistulas are successfully fixed in 84 to 99 percent of women who have surgery. If you have vaginal atrophy or are postmenopausal, low-dose estrogen cream may be prescribed before the surgery to heal tissue after the surgery.
Depending upon where the fistula is, the surgery may be done through an incision on your abdomen, vagina, or bladder. If the surgeon finds that the tissue near the fistula is not getting enough blood, a patch of your own tissue, called a graft or flap, may be used to help heal the fistula and the surrounding tissue. After surgery, you will likely need to wear a urinary catheter for 1 to 2 weeks, sometimes longer if healing is slow. In complex cases, the surgeon may have to construct a urinary diversion. This is a temporary structure that moves your urine away from the fistula, allowing it to heal. Your doctor will order a special test to ensure the wound has fully healed before the catheter is removed.
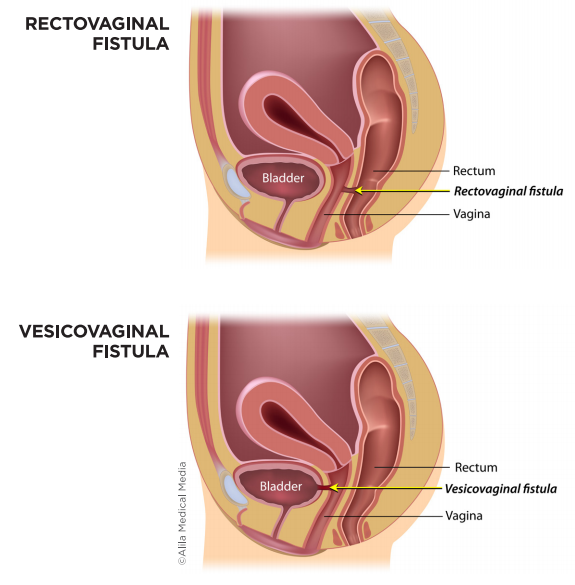
RECTOVAGINAL FISTULAS
A rectovaginal fistula is an abnormal connection in the tissue between the rectum and vagina, allowing stool to enter the vagina. Symptoms can differ from woman to woman, but most experience symptoms such as:
- Accidental bowel leakage through the vagina.
- Bad smelling discharge from the vagina.
- A sense of air escaping from the vagina.
- Recurring vaginal infections.
- Rectal or vaginal bleeding.
DIAGNOSIS OF RECTOVAGINAL FISTULAS
Your medical provider will ask you about your symptoms and when they started. If you have had surgery before, it is helpful to get the operative surgery report to know exactly what type of surgery was done.
A thorough pelvic exam will be performed to check your vagina, perineum (the skin between your vagina and your anus), anus, and rectum. Fistulas can range in size and shape–they may be twisted or straight. Sometimes, a thin metal probe is used to help find the fistula or trace out its path. Dye studies using blue-colored liquid or charcoal tablets may be needed to confirm the fistula, especially if it is small. Additional tests may be needed to assess the anal sphincter muscles. Imaging tests such as a CT scan, ultrasound, MRI, or colonoscopy may be needed to check for additional fistulas.
TREATMENT OF RECTOVAGINAL FISTULAS
Depending on the cause, size, and location of the fistula, your doctor may suggest waiting to see if the fistula heals on its own. This waiting time allows any inflammation around the fistula to improve and, if needed, increases the odds of a successful surgery. If you have inflammatory bowel disease, medicines may help to heal the fistula.
The success rate for rectovaginal fistula surgery is 90 to 95 percent. After assessing the best approach, the surgeon may perform the fistula repair through the vagina or anus. At times, a graft or tissue flap is needed to help the tissues around the fistula heal. For large fistulas, the bowel may be temporarily diverted to a bag (called an ostomy). By preventing the stool from passing through, the fistula and surrounding tissue can heal.
After the surgery, eat a healthy diet and take it easy. Learn how to clean and care for the surgical site. Avoid sexual activity, douching, or tampons until your surgeon says these things are OK. Ask your surgeon about whether you need to take antibiotics or stool softeners. To help ensure you heal properly, your goal is to produce soft, formed stools. Both constipation and diarrhea increase your risk that the wound may become infected or the repair disturbed.
If you have a temporary ostomy bag, ask for a referral to a registered dietitian to learn about any changes you’ll need to make to your diet. You will also need to meet with an ostomy nurse specialist to learn how to best care for your tissues.
LEARN THE TERMS
- Catheter: A plastic tube temporarily placed to drain urine from your bladder.
- Computerized tomography (CT) scan: A specialized type of x-ray that takes pictures of organs, blood vessels, and soft tissues from various angles.
- Genitourinary fistula: A tubular connection or tunnel in the tissue between the vagina or uterus and the urethra, bladder, or ureter.
- Perineal tear: Tearing of the perineum’s skin and/or underlying muscles during vaginal delivery, which sometimes involves the anal sphincter.
- Rectovaginal fistula: A connection or tunnel between the rectum and vagina, allowing stool to enter the vagina.
- Retrograde pyelogram: X-ray of the bladder, ureters, and kidneys.
- Ureter: The tube-like structure that runs from each kidney into the bladder, carrying urine.
- Urethra: The tube-like structure that allows urine to flow from the bladder to the outside of the body.
- Vaginal atrophy: Thinning, drying, and irritation of the lining of the vagina caused by low levels of estrogen.
- Vesicovaginal fistula: A connection or tunnel between the bladder and vagina, allowing urine to enter the vagina.
THREE TAKEAWAYS
1. Genitourinary fistulas are abnormal connections between the vagina or uterus and the urethra, bladder, or ureter. This type of fistula allows urine to flow from the urinary tract to the vagina, often causing urinary leakage.
2. Rectovaginal fistulas are connections between the rectum and vagina, allowing gas and stool to pass Into the vagina.
3. Treatment options depend on the cause, size, and location of the fistula. Surgery is not always required. Some fistulas heal on their own with time. The success rate for fistula surgery is very high. Most women experience a complete recovery.