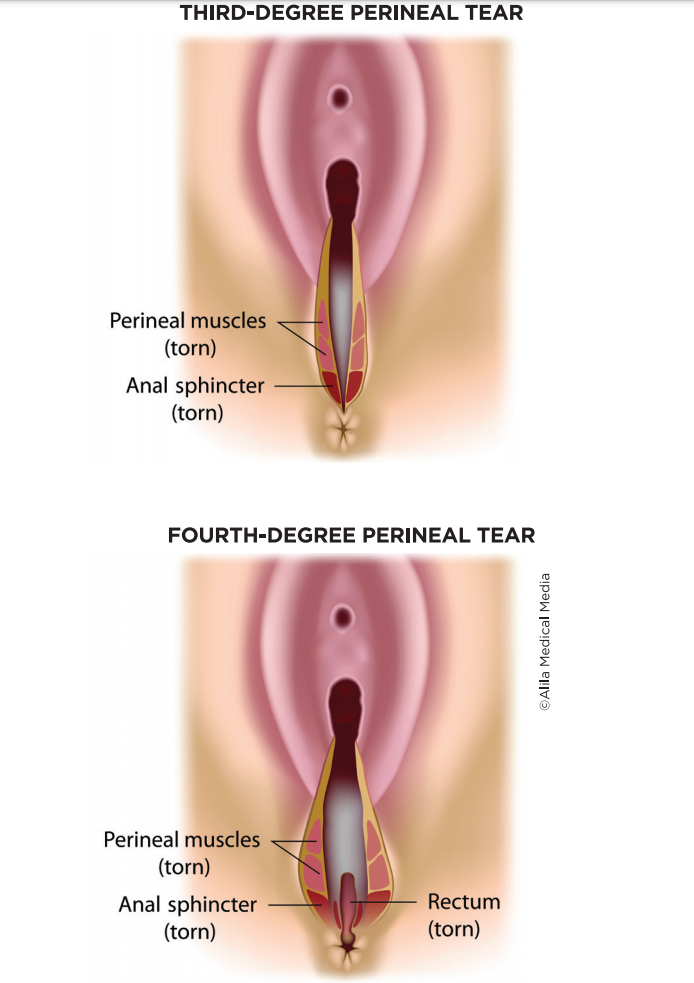
Perineal tears are damage to the area between the vaginal opening and anus that occur during vaginal delivery and have a range of severity.
About Perineal Tears
The tissue between the vaginal opening and anal opening, called the perineum, is the intersection of several muscles. Though it is designed to stretch during labor prior to delivery, perineal tears are common. They occur in more than 90 percent of women having their first vaginal delivery. These obstetrical tears are categorized into four main groups:
Third or fourth-degree perineal tears can happen to anyone. About 2 percent of women experience these types of tears. Risk factors include:
- First vaginal delivery.
- Delivery of babies weighing more than eight pounds.
- Assisted deliveries especially using forceps or a vacuum device.
- An episiotomy is performed at the time of the current or any previous delivery.
- Babies born with the face looking upward (called “OP” or occiput posterior position).
- Pushing for many hours before delivery.
- Genetics, such as having a short perineum or weak tissue.
LEARN THE TERMS
Perineum: The tissue (skin and muscles) located between the vagina and the anus.
Perineal tear: Tearing of the perineum’s skin and/or underlying muscles during vaginal delivery, which sometimes involves the ana sphincter.
Obstetrical tear: Another name for perineal tears that occur during childbirth.
Anal sphincters: Two muscles (external and internal sphincters that form a band around the anus and allow one to hold in gas and stool.
Episiotomy: Surgical cut made in the perineum just before vaginal delivery to enlarge the vaginal opening and help the baby come out.
Accidental bowel leakage: Leakage of stool (fecal incontinence) or leakage of stool and gas (anal incontinence).
Your doctor will further categorize your tear:
THIRD-DEGREE PERINEAL TEARS:
3A: less than 50 percent of the external anal sphincter is damaged.
3B: more than 50 percent of the external anal sphincter is damaged.
3C: all of the external anal sphincter and also the internal anal sphincter is damaged.
FOURTH-DEGREE PERINEAL TEARS:
Involve the external and internal anal sphincters and extend through the anal mucosa, which is the inner lining of the anus.
Having a Repair
Most of the time, your obstetrician will repair a perineal tear in the same room where you delivered. If you had an epidural, it usually provides adequate anesthesia for the repair. If not, the area will be numbed using local anesthesia. The obstetrician repairs the tear with stitches. All of the stitches will dissolve with time. They do not need to be taken out. Sometimes, you will be moved into an operating room to provide better pain control for you or, better positioning to help your doctor do the best repair possible.
While most women fully recover, some women have trouble healing or develop additional problems. About 20 percent of women experience:
- Infections or poor wound healing.
- Pain at the site of the tear (even after the skin has healed).
- Other pelvic floor symptoms such as urinary and anal incontinence.
All of these issues can be successfully treated, so stay in touch with your obstetrician. Specialized physical therapy that focuses on the pelvic floor muscles can be helpful for many of these issues. Rarely, additional procedures are required.
What to Expect After the Repair
Right after delivery, the area with the stitches will be very sensitive. Applying ice packs can help ease the pain. You may need pain medicine for several days. Keep the area clean and dry. Urinating and having a bowel movement may be quite painful. If you have to burn with urination or feel the need to urinate often, call your obstetrician. You may have a urinary tract infection (UTI).
Breastfeeding is absolutely possible with all of this going on. Make sure your obstetrician knows you are breastfeeding because it impacts what medicines can be prescribed.
Ask your obstetrician when it is OK for you to resume: Sexual activity and pelvic floor muscle exercises.
Try to take it easy. Do not insert anything into the vagina or rectum. It may take three months or more before the pain and discomfort in the perineum go away.
There are things that you can do to reduce the pain and help your perineum heal:
- Take a 10-minute sitz bath with warm water several times during the day.
- Use a squeezable water bottle (peri-bottle) to spray cool water over your perineum while urinating and after having a bowel movement. This will help reduce burning and also help keep the area clean.
- Apply warm compresses to the perineum to help soothe the area.
- Ask your obstetrician about a local anesthetic jelly or foam to numb the area.
- Be cautious about physical activities. Don’t strain and avoid heavy lifting.
- Sleep on your side.
- Try not to sit or stand for long periods of time. Sitting on a doughnut-shaped pillow–like the kind used for hemorrhoids–may also help.
Call your obstetrician if you smell an unpleasant odor/discharge or the area looks red and swollen. You may have an infection.
About 6 to 10 weeks after the procedure, the obstetrician will re-examine the perineum to ensure it has healed properly. If you are having problems, call for an exam sooner. You may want to ask for a referral to see a urogynecologist. Depending upon your tear’s specifics, an ultrasound may be required to confirm the muscles of the anal sphincter are healed.
Future Pregnancies
As long as everything heals well, vaginal birth is possible for future deliveries. Most women who have another vaginal delivery will not have a severe tear again. If you have accidental bowel leakage, discuss this with your obstetrician. Ask if a C-section might be best for you. To help reduce your risk for a future tear, aim for a slow and controlled vaginal delivery. This will allow the perineum to stretch. Ask your nurse and obstetrician to help you make the most effective pushes. Applying warm compresses on the perineum during the second stage of labor may also help prevent tearing.
THREE TAKEAWAYS
1. Perineal tears are damage to the area between the anus and the vagina, and have a range of severity.
2. Surgery Is sometimes required to repair the tears, and it may take several months to recover fully.
3. With pregnancies following third and fourth-degree tears, many women do choose to have vaginal deliveries. But, some opt to have a C-section to minimize future pelvic floor damage. Decide the route of delivery after discussing options with your obstetrician and/or urogynecologist.