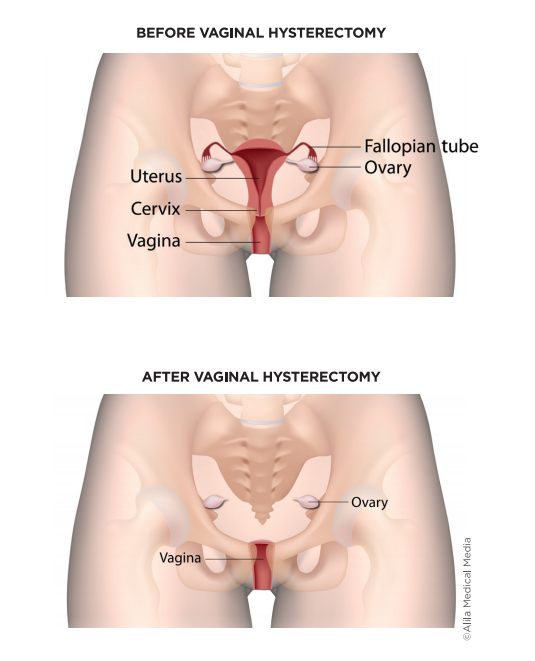
During a vaginal hysterectomy, the uterus and cervix are removed through the vagina without any abdominal incisions. This can be combined with other surgeries to fix your prolapse or incontinence. Your ovaries and Fallopian tubes might be removed at the same time.
About Vaginal Hysterectomy
Vaginal hysterectomy is a commonly performed surgery for women with prolapse. Because you do not need a large incision, most women find it easier to recover after this surgery than other forms of hysterectomy. It has the lowest complication rate of any type of hysterectomy.
Your surgeon will combine this operation with prolapse repair surgeries to address your dropped vaginal walls. It can also be performed at the same time as a surgical procedure to fix urinary incontinence.
Hysterectomy only refers to the removal of the uterus and cervix. The removal of ovaries and tubes is a different surgery called salpingo-oophorectomy, which can be performed with hysterectomy. With vaginal hysterectomy, the cervix is removed along with the uterus.
Vaginal hysterectomy is a safe surgery, but, as with any operation, there are risks. Ask your surgeon for more information about your specific risks:
- About 50 percent of women will experience a slow return of normal bladder emptying that requires the temporary use of a catheter.
- About 45 percent of women will experience a slow return of normal bowel function.
- About 10 percent of women will experience changes in bowel or bladder function.
- About 7 percent of women will experience urinary tract infections (UTIs).
- Less than 5 percent of women will experience pelvic pain, including pain with sexual activity.
- Infection of vaginal incisions and possibly the skin near the vaginal opening occurs in about 1 percent of women.
- Blood clot formation in the legs (deep vein thrombosis-DVT) or lungs (pulmonary embolus-PE) occurs in less than 1 percent of women.
- Bleeding requiring transfusion or damage to nearby organ occurs in less than 1 percent of women.
- Bowel obstruction occurs in less than 1 percent of women.
Ensure you have all your questions answered ahead of time and know how to contact your surgeon with questions or problems after surgery.
For more about preparing and recovering from urogynecological surgeries, ask your doctor’s office for a copy of the “Surgery: What to Expect” fact sheet.
How the Surgery Is Performed
This surgery can be done under general anesthesia, which means you will be asleep during surgery with a tube in your throat. It can also be done under spinal anesthesia, which means you would be numb from the waist down but breathing on your own. Discuss these choices with your surgeon, medical doctor, and anesthesia team.
During the operation, you will lie with your legs up in stirrups, similar to the position you would be in for a pelvic exam in the office. A catheter will be placed in your bladder after you are numb or asleep. The surgeon makes an incision in your vaginal wall to gain access to the abdominal cavity. This is done in a circular fashion around the cervix.
Next, the doctor carefully moves the bladder and bowel away from the uterus. The blood vessels and tissues around the uterus are detached and sealed closed with sutures or cautery. Your uterus is also detached from the ovaries and Fallopian Tubes. The surgeon removes the uterus and uses absorbable stitches to control bleeding. The top of the vaginal canal is sewn closed somewhat like the toe of a sock.
Sometimes, the Fallopian tubes and ovaries are also removed during a vaginal hysterectomy. This is called a salpingo-oophorectomy. Typically the ovaries are left in place until well after menopause to maintain hormone production. Other operations to correct pelvic floor disorders may be done at the same time, such as procedures to address urinary incontinence or to support the vaginal walls if they are prolapsed. The top of the vagina will be anchored to pelvic ligaments to fix the prolapse. Your surgeon may also look inside the bladder with a small camera to ensure nothing was damaged.
After the operation, you will be in a recovery room for a couple of hours. Some women can go home the same day after this surgery. If you have additional procedures done simultaneously, you may stay one night in the hospital. When you wake up, a catheter may be in your bladder, and you may have gauze material in the vagina. The gauze will be removed, and your bladder will be tested to see if it is ready to empty on its own before you leave the hospital. As many as 50 percent of women have trouble emptying the bladder immediately after this surgery. You may need to go home using a catheter, either placing one yourself intermittently or having it in place all the time. If so, a nurse will teach you how to do this. Ask your surgeon about when you can stop using the catheter.
Discharge Considerations
Most women recover well from this surgery and find relief from the symptoms of prolapse. Give yourself time to heal over the next six weeks. You may notice spotting and discharge from your vagina. This is normal. If the discharge has a foul odor or there is heavy bleeding, call your doctor’s office. Constipation is also very common after surgery. You will likely need the help of stool softeners and laxatives for a short time.
Avoid lifting anything heavier than you can easily lift with one hand for 6 weeks after surgery. Stay active. You can do light activities, and walking is good for you. There is no need to avoid stairs. Don’t stay in bed all the time, but refrain from high-impact exercises, swimming, spa baths, and sexual intercourse. Once you feel your reflexes are back to normal and you are not using narcotic pain medicines, you can drive.
Ask your surgeon when you should schedule a postoperative appointment. Discuss at that visit when to resume your regular activities.
THREE TAKEAWAYS
1. Vaginal hysterectomy is an operation to remove the uterus and cervix through the vaginal canal. No abdominal incisions are made. It can be combined with other operations to fix prolapse and urinary incontinence.
2. Removal of the ovaries and tubes can also be done at the same time.
3. Most women recover well from this surgery in about six weeks. Avoid high-Impact exercise, sexual activity, and heavy lifting after surgery for at least six weeks. It is normal to notice spotting and discharge from your vagina. Use stool softeners and laxatives to keep your bowels soft and regular.